Telehealth Challenges: Regional Differences Between North America and Europe
Barriers to telehealth adoption are defined by regional challenges. Here’s where North America and Europe differ and what they can learn from each other.
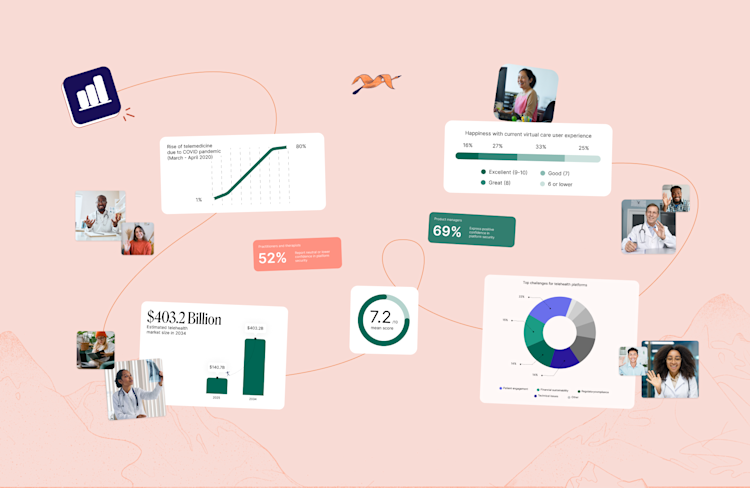
As virtual care becomes a permanent part of modern healthcare delivery, regional differences are shaping the barriers to adoption.
Insights from our State of Virtual Care Report reveal that while both North America and Europe are advancing virtual care, the barriers they face and the priorities they focus on have some clear differences.
For companies scaling telehealth across borders, these regional differences shape regulatory risk, time-to-market, and long-term growth. Organizations that adapt to local realities accelerate adoption and build durable partnerships. Those that apply a one-size-fits-all approach risk compliance setbacks, delayed revenue, and longer time to scale.
Here’s where North America and Europe differ in telehealth challenges and what they can learn from each other.
1. Limited access to technology is a major adoption problem in America
In North America, more than half of respondents (51%) identified limited access to technology and hardware as a major obstacle to patient adoption. Only 39% of European respondents said the same.

The implications of this number are significant. It means that for a substantial portion of North American telehealth providers, telehealth adoption is a question of whether patients even have the means to join in. In underserved communities, this might mean patients relying on shared devices at libraries or community centers, or providers needing to supply tablets or hotspots directly.
When a patient's only internet access is through a mobile hotspot with an inconsistent signal, even the best telehealth platform will struggle.
This is a critical consideration for telehealth platform design. Low-bandwidth optimization, asynchronous communication features, and audio-only options are baseline requirements for equitable access in North America.
2. Europe considers patient trust as a major telehealth adoption problem
A striking 50% of European respondents cited lack of patient trust in telehealth as a key barrier, compared to the 28% who flagged it as a concern in North America.

This suggests that while infrastructure may be more consistent, skepticism around the value or quality of virtual care remains a critical challenge. Patients may question:
Whether telehealth offers the same standard of care as in-person care.
Data privacy protections around digital health data
The long-term legitimacy of digital-first healthcare models
Many European healthcare cultures carry deep institutional weight where the in-person GP visit is equal to care. So, asking patients to accept a video call as equivalent takes more than a good platform. It takes a genuine shift in what people believe quality care looks like. This is why there might be some resistance to change.
For telehealth platforms operating in these environments, trust must be intentionally designed. From clear pre-visit communication to clinician presence, continuity, and privacy reassurance, experience design plays a critical role in overcoming skepticism. We’ve outlined practical strategies for building patient trust in virtual care here.
3. The compliance and regulatory pressures are different
One of the findings from our report was that European respondents were more likely to cite regulatory compliance as a major telehealth challenge (18%) compared to 11% in North America.

This likely reflects the weight of frameworks like GDPR and other data protection in Europe, which can carry substantial financial and reputational penalties for non-compliance.
In North America, the regulatory picture is also complex but different. There are several federal and state-level rules HIPAA being the dominant one) that can create confusion. So, the penalties have historically been applied more selectively.
The result is that North American organizations often operate with comparatively lighter oversight, while European providers function in an environment of heightened regulatory and public scrutiny.
That scrutiny, however, can be an advantage. European telehealth platforms that choose regionally aligned technology partners like Whereby and embed privacy-by-design into their infrastructure can turn compliance into a trust signal.
4. Data security concerns are higher in America
On data security and privacy, North America takes the lead in concern, with 16% of respondents citing it as a major challenge, compared to just 10% in Europe.

This might seem counterintuitive given Europe's GDPR reputation, but it makes a certain kind of sense. In many European markets, the regulatory infrastructure around data protection has been established long enough that compliance processes are more embedded. Organizations know what's expected and have built systems accordingly.
Although regulations like HIPAA govern patient data, in North America, particularly in the US, the heightened concern may reflect the frequency of high-profile data breaches and ransomware attacks across U.S. healthcare systems in recent years.
There's also a growing awareness among patients about how their health data might be used or monetized, which puts pressure on providers to demonstrate robust security postures.
5. Technical reliability is a bigger issue in North America
Data from our report shows that European respondents were twice as likely as their North American counterparts to report that they or their users never experience technical difficulties with telehealth (11% vs 5%).

While our survey did not probe the root causes, the reasons are likely structural. Europe generally benefits from more consistent broadband infrastructure across urban and rural areas.
In North America, the digital divide is more pronounced as rural communities, in particular, can face low bandwidth scenarios and significant connectivity challenges.
Technical reliability is foundational to patient satisfaction and provider confidence. So even small differences in connectivity or hardware access can significantly influence telehealth adoption rates.
What North American and European Regions Can Learn From Each Other
Despite their differences, both regions have valuable lessons to share. Here’s what they can each take away from each other:
What North America can learn from Europe’s telehealth approach
Embedding a privacy-first approach and compliance transparency can help patients trust digital health more.
There needs to be more consistent regulatory frameworks across North America to reduce fragmentation.
Platforms should proactively design for real-world scenarios. For example, optimizing for unstable connections, offering seamless device switching, and minimizing friction in joining calls can improve both patient satisfaction and provider confidence regardless of broader infrastructure constraints.
What Europe Can Learn From North America’s Telehealth Approach
Cybersecurity threats evolve rapidly. North America’s experience with high-profile healthcare breaches reinforces the need for ongoing investment in cyber resilience, transparent security practices, and clear communication with customers about how data is protected.
Designing for inclusion is a competitive advantage. Building lightweight, intuitive, and device-agnostic virtual care experiences ensures platforms remain accessible as they scale across diverse patient populations.
Competitive pressure in North America has also pushed telehealth platforms to clearly demonstrate ROI and prioritize user experience. European providers can benefit from more explicitly quantifying value.
Wrapping Up
In North America, access to devices, connectivity gaps, and cybersecurity risks remain central challenges. In Europe, infrastructure may be more consistent, yet patient trust and perceptions of care quality present a different kind of barrier.
These differences reinforce that scaling virtual care requires more than strong technology. It requires understanding the structural realities, regulatory environments, and cultural expectations that shape how patients and providers engage with digital health.
Organizations that recognize these nuances and adapt their strategies accordingly will be better positioned to build sustainable, trusted telehealth systems on both sides of the Atlantic.
To see job-related telehealth insights and overall priorities for the future, read the full report on the state of virtual care.